Staffing Resource Use: Medications for Opioid Use Disorder Cost Impact Model in Carceral Facilities MOUD Cost Impact Model in Carceral Facilities
Abstract
Aims
Medications for opioid use disorder (MOUD) are not widely available within United States carceral settings despite the high prevalence of opioid use disorder. Financial barriers, including staff shortages, represent common obstacles to implementation. A nationally representative survey found that among jails not providing MOUD, nearly half cited inadequate staffing as the primary reason. The purpose of this study was to develop a cost impact model to assess staffing time and costs associated with administering different forms of MOUD within carceral settings.
Materials and Methods
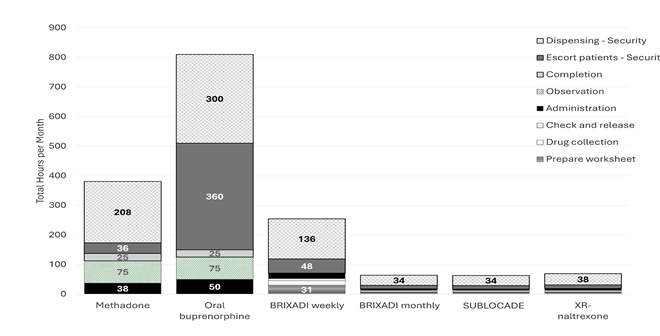
A cost impact model was developed in Microsoft Excel to simulate staff time required to administer MOUD within carceral settings. The model compared methadone, oral buprenorphine, extended-release buprenorphine (BUP-XR; SUBLOCADE* monthly and BRIXADI* weekly or monthly injectable formulations), and extended-release naltrexone (XR-NTX) for treatment of 100 incarcerated individuals per month. Information on clinician and security officer time and responsibilities was compiled using expert opinion, targeted literature reviews, prescribing information, and timestamps from manufacturer MOUD administration videos. Total staffing costs were calculated using a micro-costing approach with US Bureau of Labor Statistics national mean hourly wages for licensed practical nurses and correctional security officers.
Results
The model estimated that monthly SUBLOCADE reduced total staffing hours by 318 hours compared to methadone, 747 hours compared to oral buprenorphine, 192 hours compared to weekly BRIXADI, 1 hour compared to monthly BRIXADI, and 6 hours compared to XR-NTX per 100 patients per month. Corresponding monthly staffing cost reductions ranged from $23 to $22,148 compared to other MOUD formulations.
Limitations and Conclusions
Limitations include reliance on assumptions for certain administration times and escorting procedures, and exclusion of medication acquisition costs. Despite these limitations, long-acting injectable buprenorphine formulations reduce total staffing time and costs compared to other MOUD, potentially helping relieve the operational capacity burden that represents a major institutional barrier to MOUD program implementation in carceral settings.
Full text article
References
Scott CK, Dennis ML, Grella CE, et al. The impact of the opioid crisis on U.S. state prison systems. Health Justice [Internet]. 2021;9(1):17.
Cases involving discrimination based on treatment with medication for opioid use disorder (moud) [Internet]. 2025. Available from: https://www.lac.org/assets/files/Cases-involving-denial-of-access-to-MOUD.pdf.
Cariappa P, LaFarge E, Threatte L, et al. Your right to adequate medical care. Available from: https://jlm.law.columbia.edu/files/2021/02/30.-Chapter-23.pdf.
Longley, Joseph Weizman, Shelly Brown, Somer LaBelle, Regina. A National Snapshot Update: Access to Medications for Opioid Use Disorder in U.S. Jails and Prisons [Internet]. Georgetown Law Center; 2023 [cited 2025 Dec 27]. Available from: https://oneill.law.georgetown.edu/publications/a-national-snapshot-update-access-to-medications-for-opioid-use-disorder-in-u-s-jails-and-prisons/.
Flanagan Balawajder E, Ducharme L, Taylor BG, et al. Factors associated with the availability of medications for opioid use disorder in US jails. JAMA Netw Open [Internet]. 2024 [cited 2025 Dec 27];7(9):e2434704.
Howell BA, Martin RA, Lebeau R, et al. Changes in health services use after receipt of medications for opioid use disorder in A statewide correctional system. Health Affairs [Internet]. 2021 [cited 2025 Dec 27];40(8):1304–1311.
Prison Health Care: Costs and Quality [Internet]. The Pew Charitable Trusts; 2017. Available from: https://www.pew.org/~/media/assets/2017/10/sfh_prison_health_care_costs_and_quality_final.pdf.
Governor’s Budget Summary: Criminal Justice and Judicial Branch [Internet]. CALIFORNIA DEPARTMENT OF CORRECTIONS AND REHABILITATION; 2025. Available from: https://ebudget.ca.gov/2025-26/pdf/BudgetSummary/CriminalJusticeandJudicialBranch.pdf.
Texas Department of Criminal Justice. Fiscal Year 2025 Operating Budget [Internet]. Texas Department of Criminal Justice; 2024. Available from: https://www.tdcj.texas.gov/documents/bfd/LAR_FY2026-27_Board_Document.pdf.
Khairat S, Zebrowski A, Stabile K, et al. Assessment of stakeholder perceptions and cost of Implementing a telemedicine specialty program at correctional facilities in North Carolina. Perm J [Internet]. 2023;27(3):49–59.
Ryan D, Ekanayake DL, Evans E, et al. Cost analysis of MOUD implementation and sustainability in Massachusetts jails. Health Justice [Internet]. 2025;13(1):9.
Jalali A, Jeng PJ, Polsky D, et al. Cost-effectiveness of extended-release injectable naltrexone among incarcerated persons with opioid use disorder before release from prison versus after release. J Subst Abuse Treat [Internet]. 2022;141:108835.
Opioid Use Disorder Treatment in Jails and Prisons [Internet]. The Pew Charitable Trusts; 2020. Available from: https://www.pew.org/-/media/assets/2020/04/caseformedicationassistedtreatmentjailsprisons.pdf.
Lim S, Cherian T, Katyal M, et al. Association between jail-based methadone or buprenorphine treatment for opioid use disorder and overdose mortality after release from New York City jails 2011-17. Addiction [Internet]. 2023;118(3):459–467.
Lim S, Cherian T, Katyal M, et al. Jail-based medication for opioid use disorder and patterns of reincarceration and acute care use after release: A sequence analysis. J Subst Use Addict Treat [Internet]. 2024;158(209254):209254.
Cherian T, Lim S, Katyal M, et al. Impact of jail-based methadone or buprenorphine treatment on non-fatal opioid overdose after incarceration. Drug Alcohol Depend [Internet]. 2024 [cited 2025 Dec 27];259(111274):111274.
Will J, Abare M, Olson M, et al. Emergency department utilization by individuals with opioid use disorder who were recently incarcerated. J Subst Abuse Treat [Internet]. 2022;141(108838):108838.
Ryan DA, Montoya ID, Koutoujian PJ, et al. Budget impact tool for the incorporation of medications for opioid use disorder into jail/prison facilities. J Subst Use Addict Treat [Internet]. 2023;146:208943.
U.S. Bureau of Labor Statistics. Occupational Employment and Wage Statistics [Internet]. 2024 [cited 2025 Dec 27]. Available from: https://www.bls.gov/oes/tables.htm.
Occupational Employment and Wage Statistics (OEWS) Tables: 33-3012 Correctional Officers and Jailers [Internet]. US Bureau of Labor Statistics. 2023 [cited 2025 Dec 27]. Available from: https://www.bls.gov/oes/2023/may/oes333012.htm.
Ferguson WJ, Johnston J, Clarke JG, et al. Advancing the implementation and sustainment of medication assisted treatment for opioid use disorders in prisons and jails. Health Justice [Internet]. 2019;7(1):19.
Berk J, South A-M, Martin M, et al. Medication for opioid use disorder service delivery in carceral facilities: update and summary report. Health Justice [Internet]. 2025;13(1):8.
Russell C, George TP, Chopra N, et al. Feasibility and effectiveness of extended-release buprenorphine (XR-BUP) among correctional populations: a systematic review. Am J Drug Alcohol Abuse [Internet]. 2024;50(5):567–586.
Woods A, Foley C, Conigrave KM, et al. Extended-release pharmacotherapies for substance use disorders in incarcerated populations: A systematic review. Addiction [Internet]. 2025;120(5):835–859.
Wong JSH, Masson S, Huang A, et al. Cost analysis of buprenorphine extended-release injection versus sublingual buprenorphine/naloxone tablets in a correctional setting. J Correct Health Care [Internet]. 2022;28(6):368–371.
Chatterjee A, Weitz M, Savinkina A, et al. Estimated Costs and Outcomes Associated With Use and Nonuse of Medications for Opioid Use Disorder During Incarceration and at Release in Massachusetts. JAMA Netw Open [Internet]. 2023;6(4):e237036.
Horn BP, Li X, McCrady B, et al. Cost-effectiveness analysis of a large jail-based methadone maintenance treatment continuation program in New Mexico. J Subst Abuse Treat [Internet]. 2020;115:108042.
Zarkin GA, Orme S, Dunlap LJ, et al. Cost and cost-effectiveness of interim methadone treatment and patient navigation initiated in jail. Drug Alcohol Depend [Internet]. 2020;217:108292.
Rich JD, McKenzie M, Larney S, et al. Methadone continuation versus forced withdrawal on incarceration in a combined US prison and jail: a randomised, open-label trial. Lancet [Internet]. 2015;386(9991):350–359.
How to Administer Brixadi [Internet]. US: Braeburn Inc.; 2024 [cited 2025 Dec 27]. Available from: https://www.brixadihcp.com/dosing-and-administration/administering-brixadi/.
Indivior UK Limited. SUBLOCADE administration and storage [Internet]. 2025 [cited 2025 Dec 27]. Available from: https://www.sublocadehcp.com/resources#ifu-video.
Understand how to prepare and administer once-monthly VIVITROL [Internet]. US: Alkermes Inc.; 2023 [cited 2025 Dec 27]. Available from: https://www.vivitrolhcp.com/preparation-and-administration.
Authors
Copyright (c) 2026 Chris Poole, Courtney Flynn, Kristin Kistler, Stephen Chaplin, Joris van Stiphout, Rashad Carlton, Meghan Thompson, Jessica Jay, William Mullen

This work is licensed under a Creative Commons Attribution 4.0 International License.